
Simultaneous herpes zoster rash in the upper extremity and interscapular region that resembles innervation zone of the dorsal ramus of the cervical nerve root: a case report
Introduction
Cervical radiculopathy is the clinical description of a condition in which a nerve root in the cervical spine becomes inflamed or damaged, resulting in a change of neurological function. Radiculopathy rarely occurs from spontaneous neurogenic inflammation, and it is commonly caused by compression of the cervical nerve root by a substance from a herniated intervertebral disc or arthritic bone spur in the cervical foramen by degenerative alteration. It leads to radicular pain, sensational disturbance, and motor dysfunction along the nerve’s pathway into the upper extremity on the ipsilateral side, corresponding to a dermatome pattern (1). In addition, neck or scapular pain is commonly seen before the onset of pain in the upper extremity during cervical radiculopathy (2,3). Although a previous article reported cervical nerve root involvement in cervical radiculopathy as the origin of neck or scapular pain, the cause of the pain had been uncertain (4). The aim of this report is to present a case of herpes zoster with simultaneous skin rash in the upper extremity and interscapular region. To the best of our knowledge, this is the first report to visualize the innervation zone of the medial branches of the dorsal ramus of the cervical nerve root on the scapula, which corresponds to the painful scapular region in cases of cervical radiculopathy.
We present the following case in accordance with the CARE reporting checklist (available at http://dx.doi.org/10.21037/acr-21-1).
Case presentation
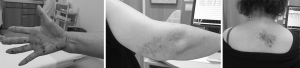
A 71-year-old healthy woman presented to our clinic with sudden shoulder pain on the right side without any traumatic episodes. She had no major medical history, and no immunodeficiencies were noted. On initial physical examination, she had motion pain and stiffness on the right shoulder, the painful arc test was positive at 90° of abduction, and the Hawkins sign was positive (5). Radiological examination showed no abnormality of the shoulder, and on the basis of these findings, non-calcific tendonitis of the rotator cuff was first suggested, and then she was treated with triamcinolone acetonide injection into the subarachnoid space. She was transiently relieved from the shoulder pain for 3 days, and afterward, she repeatedly suffered from shoulder and scapular pain associated with neuralgia in the upper extremity on the right side. On the second physical examination, Jackson’s test and Spurling’s test showed positivity for scapular pain and neuralgia, which was similar to the symptom of cervical radiculopathy (1). At the same time, she had a blistering skin rash on the ulnar side of her upper extremity and interscapular region on the right side (Figure 1). She was referred to a dermatologist, who diagnosed this rash as herpes zoster and prescribed oral amenamevir and topical vidarabine ointment for 7 days. Her neuralgia continued after the disappearance of the skin rash and oral treatment with 300 mg/day pregabalin for 14 days, and she was treated by a pain physician. After 1 year, she presented with mild postherpetic neuralgia of the 3rd to 5th fingers of the right hand and required 75 mg/day oral pregabalin.
A copy of the written consent is available for review by the Editor-in-Chief of the journal. All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional research committee and with the Helsinki Declaration (as revised in 2013).
Discussion
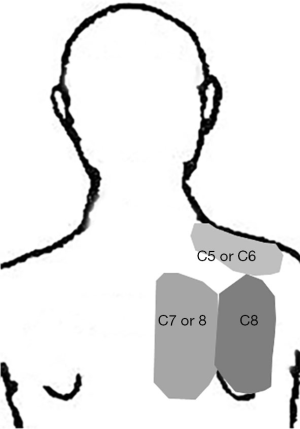
Cervical radiculopathy is often accompanied by neck or scapular pain on the backside (2,4). In 2006, Tanaka et al. demonstrated a distinct clinical relationship between the region of scapular pain and each study indicated a level of the involved nerve root in cervical radiculopathy (4). They showed that scapular pain occurs in the suprascapular, interscapular, and scapular regions, which correspond to C5 or C6, C7 or 8, and C8 cervical radiculopathy, respectively (Figure 2). Indeed, this report is so accurate that the level of the compressed nerve root from the region of the associated scapular pain in clinical situations to treat cervical radiculopathy is predictable. To clarify the cause of the scapular pain, Mizutamari et al. attempted an anatomical study to reveal scapular pain secondary to cervical radiculopathy arising from the medial branches of the dorsal ramus of the individual spinal nerve roots (2). They found that the C5 and C8 dorsal ramus changed to a cutaneous nerve, gradually descending inferolaterally to the suprascapular region and to the middle of the scapular region, respectively; however, they found no C6 or C7 dorsal ramus descending to the scapular region, and it seemed incomplete enough to confirm the distinct mechanism of the scapular pain secondary to cervical radiculopathy. In the current case, there was a blistering skin rash of herpes zoster on the ulnar side of her upper extremity and interscapular region. In case of herpes zoster originating from the spinal dorsal root ganglia, reactivated varicella zoster virus (VZV) typically travels from the individual single ganglia along the sensory nerves to the skin, causing prodromal pain followed by eruption of the rash (6), as there is no anatomical communication among the ganglia in the spine. It seems that the rash in the upper extremity and interscapular region is caused by VZV traveling from the same ganglion, probably from the C8 ganglion, considering the dermatome of the rash region in the upper extremity corresponds to the scapular region related to C7 or C8 cervical radiculopathy, as illustrated by Tanaka et al. in 2006 (4). There is little possibility of a rash in the interscapular region originating from the thoracic spinal root ganglion because the rash pattern is not linear along the intercostal nerve. Thus, our findings are important for visualizing the innervation zone of the medial branches of the dorsal ramus of the C8 cervical nerve root on the scapula, implying that scapular pain occurs in cases of cervical radiculopathy.
Skin rash due to reactivation of herpes zoster is commonly seen in the thoracic dermatomes and cranial nerves, and it is relatively rare in cervical dermatomes (7-11). There are a few case reports of herpes zoster in the upper extremity, particularly in ulnar nerve distribution (7,9-11), which are similar to our case; however, to our knowledge, no study has reported a rash in the simultaneous interscapular region. One possibility is that no clinician can imagine skin rash in the scapular region and ulnar nerve innervation in the upper extremity originating from the same ganglion of the cervical spine because of the large distance between the two regions. Another possibility is that VZV traveling along the medial branches of the dorsal ramus of the cervical nerve root causing skin rash in the interscapular region itself is extraordinary; thus, our case is the first report on this phenomenon.
In the current case, amenamevir is used for the treatment of herpes zoster. Amenamevir, a herpesvirus helicase-primase inhibitor, has been used for the treatment of herpes zoster in Japan since 2017 (12). It has a different action mechanism from previously approved synthetic nucleoside compounds for the treatment of herpes zoster, including acyclovir, valacyclovir, and famciclovir. The usual adult dose is 400 mg amenamevir p.o. once daily for 7 days. The benefit is its ability to cure herpes zoster as well as prevent postherpetic neuralgia (12); however, in the current case, the patient still had mild postherpetic neuralgia after 1 year, and she still needed oral pregabalin treatment.
In conclusion, a case of herpes zoster with simultaneous skin rash in the upper extremity and interscapular region was reported. The interscapular region illustrated by the skin rash corresponded to the innervation zone of the medial branches of the dorsal ramus of the cervical nerve root, which resembled the scapular region in the case of C8 cervical radiculopathy. However, further case reports are required to confirm this unique phenomenon.
Acknowledgments
Funding: None.
Footnote
Reporting Checklist: The authors have completed the CARE reporting checklist. Available at http://dx.doi.org/10.21037/acr-21-1
Peer Review File: Available at http://dx.doi.org/10.21037/acr-21-1
Conflicts of Interest: Both authors have completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/acr-21-1). Both authors have no conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. Written informed consent was obtained from the patient for publication of this case report and any accompanying images. A copy of the written consent is available for review by the Editor-in-Chief of the journal. All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional research committee and with the Helsinki Declaration (as revised in 2013).
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Eubanks JD. Cervical radiculopathy: nonoperative management of neck pain and radicular symptoms. Am Fam Physician 2010;81:33-40. [PubMed]
- Mizutamari M, Sei A, Tokiyoshi A, et al. Corresponding scapular pain with the nerve root involved in cervical radiculopathy. J Orthop Surg (Hong Kong) 2010;18:356-60. [Crossref] [PubMed]
- Willeford M, Willeford S. Referred scapula pain from C6 or C7 cervical spinal stenosis. Open J Pain Med 2019;3:21-3. [Crossref]
- Tanaka Y, Kokubun S, Sato T, et al. Cervical roots as origin of pain in the neck or scapular regions. Spine (Phila Pa 1976) 2006;31:E568-73. [Crossref] [PubMed]
- Phillips N. Tests for diagnosing subacromial impingement syndrome and rotator cuff disease. Shoulder Elbow 2014;6:215-21. [Crossref] [PubMed]
- Reichelt M, Zerboni L, Arvin AM. Mechanisms of varicella-zoster virus neuropathogenesis in human dorsal root ganglia. J Virol 2008;82:3971-83. [Crossref] [PubMed]
- Athwal GS, Bartsich SA, Weiland AJ. Herpes zoster in the ulnar nerve distribution. J Hand Surg Br 2005;30:355-7. [Crossref] [PubMed]
- Cukic V. The Uncommon Localization of Herpes Zoster. Med Arch 2016;70:72-5. [Crossref] [PubMed]
- Hashemilar M, Ghabili K, Shoja MM, et al. Varicella-zoster virus reactivation from multiple ganglia: a case report. J Med Case Rep 2009;3:9134. [Crossref] [PubMed]
- Şalçini C, Sunter G, Gumustas SA, et al. Cervical dermatomal zona misdiagnosed as ulnar nerve entrapment. BMJ Case Rep 2015;2015:bcr2015209669 [Crossref] [PubMed]
- Kayipmaz M, Basaran SH, Ercin E, et al. Isolated ulnar dorsal cutaneous nerve herpes zoster reactivation. Orthopedics 2013;36:e1217-9. [Crossref] [PubMed]
- Shoji N, Tanese K, Sasaki A, et al. Pharmaceuticals and Medical Device Agency approval summary: Amenamevir for the treatment of herpes zoster. J Dermatol 2020;47:683-8. [Crossref] [PubMed]
Cite this article as: Nomura H, Nomura S. Simultaneous herpes zoster rash in the upper extremity and interscapular region that resembles innervation zone of the dorsal ramus of the cervical nerve root: a case report. AME Case Rep 2021;5:25.


