
Rare presentation of bilateral thumb psoriatic arthritis treated with arthrodesis: a case report
Introduction
Psoriatic arthritis (PsA) is a chronic inflammatory joint disease presenting concomitantly with scaly cutaneous abnormalities and the absence of rheumatoid factor (RF). Although a projected 1% of the population suffers from PsA, multiple studies estimate the prevalence and incidence of PsA in patients with psoriasis to be 4–30% and 3.8–8 per 100,000, respectively (1-5).
PsA consists of five main types that may contribute to destructive arthritis in multiple joints and cause significant disability. The most common variant, asymmetric PsA, is generally mild, involves fewer than three total joints, and spares the corresponding contralateral joint. In comparison, symmetric PsA makes up only a quarter of cases and presents similarly to rheumatoid arthritis, albeit with milder symptoms and reduced risk for joint deformity. Regardless of PsA classification type, hands are a common site of pathology, with studies suggesting involvement in up to 84% of cases (1,3).
While hyperextension deformities are a rare occurrence, thumb involvement in PsA typically presents as metacarpophalangeal (MP) flexion and interphalangeal (IP) extension abnormalities with associated trapeziometacarpal (TMC) joint stiffness (6). In this setting, radiographic findings typically reveal erosion and osteolytic changes associated with joint space widening and digital shortening. Although most cases are mild, PsA may progress to severely debilitating forms commonly associated with joint subluxation, however, documented frank dislocations are rare (6,7). Given the autoimmune etiology of the condition, PsA is frequently treated pharmacologically with disease-modifying anti-rheumatic drugs (DMARDs) such as methotrexate and TNF-alpha inhibitors. Due to the explosion in popularity and effectiveness of DMARDs and other medications, progression to severe disease is becoming increasingly rare. In these severe cases, surgical treatment with joint arthrodesis should be considered (8-10).
We present the following case in accordance with the CARE reporting checklist (available at http://dx.doi.org/10.21037/acr-20-136).
Case presentation
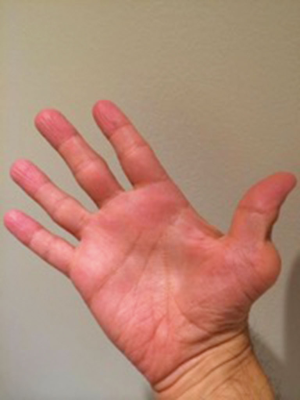
A 47-year-old male presented with an 18-year history of PsA managed medically with etanercept, leflunomide, and naproxen. At presentation he had a fifteen-year history of bilateral thumb involvement, characterized by pain, instability, dislocation, and loss of function. Physical examination of the right hand revealed joint tenderness and effusion of the first through third MP and second through fourth PIP joints. The right thumb also demonstrated laxity with passive stress in all directions, as well as, dislocation of the MP joint and hyperextension of the IP joint (Figure 1). Further examination of the left hand revealed first through third MP joint tenderness and thumb Z-deformity with MP joint swelling.
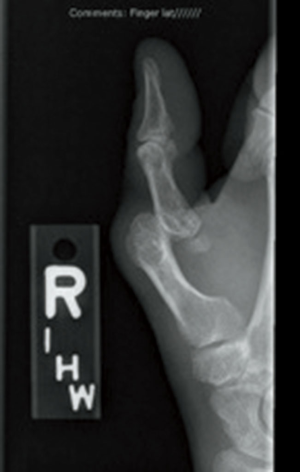
Radiographs of the right hand revealed dislocation at the right first MP joint with erosions of the first metacarpal head and base of the first proximal phalanx (Figure 2). Soft tissue calcifications at the radial aspect of the right first IP joint were also evident. In comparison, radiographs of the left hand demonstrated a flexion deformity at the first MP joint without evidence of dislocation, no erosion of the MP joint, and maintenance of the DIP joint spaces. Absence of the ulnar styloid was also suggestive bilaterally on imaging and presumably related to erosions. The decision was then made to proceed with surgery for a right thumb MP and IP joint arthrodesis.
In the operating room, the right thumb MP joint was approached volarly. The MP joint was then dislocated and the metacarpal head debrided of all cartilage. An osteotomy was performed to place the MP joint in approximately 30 degrees of flexion and the base of the proximal phalanx was debrided of sclerotic bone due to the presence of pseudoarthrosis at the dorsal margin. Using an oscillating saw, the articular margin was cut flat.
The OsteoMed hand fusion set was used during the procedure. The joint surfaces were then opposed, and a K-wire was placed antegrade from the metacarpal into the proximal phalanx. A reamer was utilized on the distal portion of the metacarpal, and a 2.0 mm plate was placed and cannulated screws applied across the joint. Three non-locking screws were applied into the shaft of the metacarpal in the plate, compressing the plate to bone. The IP joint was then approached, cartilage removed, and the joint fused with two 8-mm staples.
At one-week follow-up the patient was placed into a short arm thumb spica cast including the IP joint for one month. On examination, the MP and IP joints appeared appropriately reduced (Figure 3). The patient was then placed into a forearm-based thumb spica cast, which was removed after a month.
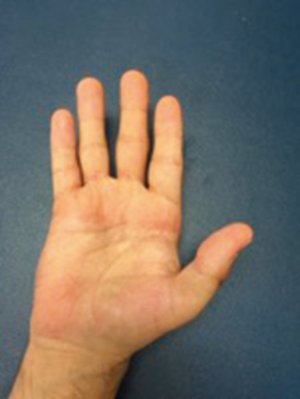
The patient was satisfied with the outcome and decided to undergo the same procedure on the contralateral thumb due to significant disability and underwent left MP and IP joint arthrodesis. Upon accessing the MP joint, the collateral ligaments were released off of the head of the metacarpal, and the head of the metacarpal was osteotomized at a 25-degree angle. The base of the thumb proximal phalanx was then excised perpendicular to the shaft, the joint surfaces were opposed, and a guidewire was inserted from the metacarpal into the proximal phalanx. After reaming, a 2.0 mm plate was then placed over the wire and a cannulated screw was applied over the guidewire, providing compression across the fusion site. Three nonlocking screws were placed in the shaft of the metacarpal in the plate, maintaining the MP joint in 20 degrees of flexion. The remainder of the surgery including fusion of the IP joint, closure, and postoperative management was treated similarly to the previous surgery.
Five months after his second surgery, the patient expressed satisfaction with the positioning of his digits and the functional mobility to use his hands asymptomatically during daily activities. Further examination also supported stability of the MP and IP joints with radially and ulnar deviated stress, as well as, fully intact sensation. Additionally, plain radiographs confirmed reduction of the MP and IP joints and hardware to be appropriately positioned (Figure 4).
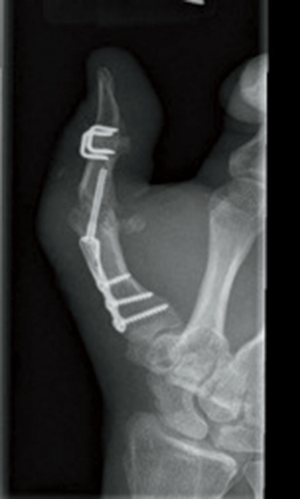
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee(s). Written informed consent was obtained from the patient.
Discussion
Although DMARDs are beneficial in patients with PsA, these agents are not without side effects. If PsA progresses to the point where medical management is considered ineffective, surgical intervention should be explored with special considerations. First, the osteotomy angle and degree of flexion the thumb was placed in was an important consideration for surgery. In this setting, increased flexion may result in higher failure rates, however, some degree of flexion is essential to allow for gripping and pinching. Second, while the use of compression screws is a well-established treatment for inflammatory arthritis and joint instability during MP joint arthrodesis, staples were used to avoid production of a stress riser in the proximal phalanx (10). Third, postoperative immobilization in a spica cast is necessary for achieving union (10).
This case is unique because the patient presented with a severely debilitating dislocation without diffuse joint erosion. On review of the literature, no similar cases have been reported. Such functional disability is typically seen in arthritis mutilans (AM), however, this patient did not fall into this classification given he had bilateral first MP joint involvement and lacked significant erosions or other clinical signs of AM. One such consideration was Jaccoud’s arthropathy, a condition with reversible MP joint subluxation resulting from fibrous contractures and capsular retraction caused by repeated bouts of arthritis, however, these patients typically lack the erosive radiographic changes seen in AM. Although this was a possible consideration in this patient with an inflammatory arthritis, no associated fibrotic changes were demonstrated. This patient most likely had a rare variant of symmetric PsA primarily involving the first MP joints severe enough to cause dislocation. Moreover, the classification in this patient was important, as cases of failed arthrodesis due to significant osteolysis have been reported in patients with AM. Although conservative treatment remains an option in AM, surgical intervention was deemed appropriate given the lack of significant erosions on imaging.
The instability of the patient’s left first MP joint was also significant given the progressive nature of disease. Given the patient had previously reported a similar presentation in his right thumb, it was presumed that his left thumb had a higher likelihood to dislocate, thus, it was reasoned the patient would benefit from an identical operation. Overall, the management of this patient highlights evidence demonstrating the efficacy of multiple joint arthrodesis to improve functionality in patients suffering from severe forms of PsA.
Acknowledgments
Funding: None.
Footnote
Reporting Checklist: The authors have completed the CARE reporting checklist. Available at http://dx.doi.org/10.21037/acr-20-136
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/acr-20-136). The authors have no conflicts to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee(s). Written informed consent was obtained from the patient.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Gladman DD, Antoni C, Mease P. at al. Psoriatic arthritis: epidemiology, clinical features, course, and outcome. Ann Rheum Dis 2005;64:ii14-17. [PubMed]
- Zachariae H. Prevalence of joint disease in patients with psoriasis: implications for therapy. Am J Clin Dermatol 2003;4:441-7. [Crossref] [PubMed]
- Gelfand JM, Gladman DD, Mease PJ, et al. Epidemiology of psoriatic arthritis in the population of the United States. J Am Acad Dermatol 2005;53:573. [Crossref] [PubMed]
- Mease PJ, Gladman DD, Helliwell P, et al. Comparative performance of psoriatic arthritis screening tools in patients with psoriasis in European/North American dermatology clinics. J Am Acad Dermatol 2014;71:649-55. [Crossref] [PubMed]
- Trail IA, Stanley JK. The hand in psoriasis. J Hand Surg Br 1990;15:79-83. [Crossref] [PubMed]
- Choo AD, Middleton G, Wilson RL. Nonrheumatoid Inflammatory Arthroses of the Hand and Wrist. J Hand Surg Am 2015;40:2477-87; quiz 2488. Erratum in: J Hand Surg Am 2016;41:576. [Crossref] [PubMed]
- Nalebuff EA. Surgery of psoriatic arthritis of the hand. Hand Clin 1996;12:603-14. [Crossref] [PubMed]
- Nystad TW, Husum YS, Furnes ON, et al. Incidence and Predictive Factors for Orthopedic Surgery in Patients with Psoriatic Arthritis. J Rheumatol 2018;45:1532-40. [Crossref] [PubMed]
- Haque N, Lories RJ, de Vlam K. Orthopaedic interventions in patients with psoriatic arthritis: a descriptive report from the SPAR cohort. RMD Open 2016;2:e000293 [Crossref] [PubMed]
- Day MS, Nam D, Goodman S, et al. Psoriatic arthritis. J Am Acad Orthop Surg 2012;20:28-37. [Crossref] [PubMed]
Cite this article as: Tanenbaum ZG, Leider JD, Ehlers CB, Apseloff NA, Ryan JA, Kessler MW. Rare presentation of bilateral thumb psoriatic arthritis treated with arthrodesis: a case report. AME Case Rep 2021;5:18.


