
Roles of specific drug therapies for severe pulmonary arterial hypertension in palliative care: a case report
Introduction
Pulmonary arterial hypertension (PAH) is an uncommon but potentially life-threatening illness. The elevated pulmonary arterial blood pressure will lead to right heart failure and even cardiopulmonary collapse if it is severe. Apart from general supportive measures, pulmonary hypertension-specific therapies (PHST) are available to slow down disease progression, but they are not curative. According to previous studies, many patients with severe PAH often had significant physical symptoms and psychological distress for both themselves and their families at the end of life. Moreover, they would have repeated admissions due to physical deterioration and decline in functioning associated with worsening in cardiac function. Some of these patients might suffer from unnecessary aggressive interventions and resuscitation because of lack of advance care planning discussion. As such, Palliative Care (PC) would be an important element as part of the overall management (1). Hereby, we present a case of severe PAH, who benefited from the use of PHST together with the input by PC team. The case report showed the collaborative work between PC and parent teams. While parent team was able to manage the medical conditions related to PAH, however the physical and psychosocial needs should be addressed by PC team. More importantly, the PC team has essential roles of providing advance care planning discussions with the patient and thus might avoid unnecessary interventions.
We present the following case in accordance with the CARE reporting checklist (available at http://dx.doi.org/10.21037/acr-20-108).
Case presentation
This 40-year-old lady with history of schizoaffective disorder on regular use of serotonin selective reuptake inhibitor (SSRI), presented with chest pain and shortness of breath in 2015. After further work-up, she was found to have severe PAH together with hypertension, hyperlipidemia, obesity, fatty liver, asthma, obstructive sleep apnoea. Echocardiogram showed preserved left ventricular function, dilated right ventricle, impaired right ventricular systolic function and pulmonary hypertension. The measured right ventricular systolic pressure was 76 mmHg. Computed tomography excluded pulmonary aetiologies (Figure 1). Right heart catheterization showed mean pulmonary arterial pressure was 52 mmHg and did not show any significant vasodilatory response after adenosine infusion. Her 6 mins walk test (6MWT) at room air was 270 meters. The diagnosis was idiopathic PAH as there was no secondary cause of PTH identified.
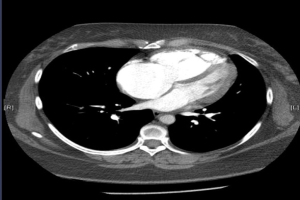
She was then started on monotherapy, sildenafil 20mg thrice daily since 2016. Anticoagulants and diuretics were also given in view of risk of thrombosis and fluid overload. Her SSRI was then stopped. However, her exercise tolerance gradually deteriorated, and she experienced more frequent near syncope. She was dyspnoeic on exertion and required long term oxygen since 2017. One of the prognostic indicators, N-terminal pro-Brain natriuretic peptide (NT-proBNP) was elevated (2,460 pg/mL; reference: >450 pg/mL). Her daily activities became limited and reached WHO class III. Because of worsening functional conditions, additional PAH-specific agents macitentan 10 mg daily and selexipag 400 microgram were given subsequently in 2017 and 2018. However, she was not a candidate for lung transplant because of severe obesity.
She had repeated admissions due to chest symptoms in 2019 and was later referred to PC team for complicated symptom management and psychosocial care. On PC team assessment, she had palpitation, anorexia, retrosternal discomfort, insomnia, fatigue and shortness of breath. She had signs of fluid overload and required oxygen therapy at 6 L/min. Chest X-ray showed congested lung field (Figure 2). Her symptoms were so distressing that she became mostly bed-bound and could not perform any physical activities. In addition, she had spiritual distress with feelings of hopeless, depressed and meaningless since curative treatment was not available for her. She was just panic about the chance of sudden death for herself and so could not sleep well. In addition, she worried about her son who had attention deficit hyperactivity disorder and her mother, who was the main carer, expressed grief about potential loss of her daughter.
Because of persistent chest symptoms, subcutaneous fentanyl infusion and midazolam were eventually required as to palliative her breathlessness and pain in hospital. She was also referred to clinical psychologist and chaplain for psychological and spiritual support. After 3–4 weeks of PC treatment, her chest symptoms were markedly reduced and there was less rumination of her negative thoughts. Her mother also joined our care-giver support group. Moreover, she started to have greater sense of control and felt less anxious because the breakthrough symptoms could now be improved with rest and our opioid treatment. As her condition became stable, subcutaneous fentanyl infusion was changed to transdermal fentanyl patch at the dose of 2.1 mg every 72 hours. With this multidisciplinary approach, she had improvement in functional class, and managed to do simple tasks of daily living with long term oxygen therapy. She can be discharged to home successfully and had regular out-patient follow-up. She was not hospitalised for 3 months already.
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee(s) and with the Helsinki Declaration (as revised in 2013). Written informed consent was obtained from the patient.
Discussion
The development of PAH specific medications is one of the major factors that account for improvement in survival in the past 2 decades. The 5-year survival rate for patients with idiopathic PAH was around 65% (2). However, they are expected to deteriorate with more and more symptoms. Just like this case, these patients usually present with chest discomfort and dyspnoea which worsen and most of them became homebound with oxygen dependent, over several years. As a result, they will develop emotional and caring problems. Eventually, both patients and their caregivers often have strong psychosocial needs. Although there is no strong evidence for early PC integration with severe PAH, the incorporation of palliative team is highly recommended (1).
In this case, she had several poor prognostic factors including signs of right heart failure, syncope, elevated NT-proBNP, 6MWT less than 300 metres and WHO functional class IV (3). Thus, she only had limited survival. In the management of PAH, conventional measures include oxygen therapy, vaccination, diuretics, anticoagulation and pulmonary rehabilitation are recommended (1). WHO functional class is commonly used for risk stratification and is an important factor to determine the use of PAH-specific therapies. In selected patients who tested positive response with acute vasoreactivity test, a trial of calcium channel blocker should be administered. In fact, there are 4 classes of PAH-specific pharmacological treatments, namely endothelial receptor antagonist (ERA), nitric oxide-cyclic guanosine monophosphate enhancers, oral prostacyclin receptor agonists and prostanoids. Both phosphodiesterase inhibitors (PDE5I) (e.g., sildenafil, tadalafil and Vardenafil), as well as guanylate cyclase stimulant (e.g., riociguat) are nitric oxide-cyclic guanosine monophosphate enhancers. They achieve vasodilation via different mechanisms. No direct comparison of effectiveness among different therapeutic agents is available. The selection of therapeutic regimen is also affected by local drug availability, cost and patient’s preference (1).
One of the most readily available PDE5Is, sildenafil, is often started as initial monotherapy in our local institution. Its efficacy on improving exercise capacity and cardiopulmonary hemodynamics had been demonstrated in randomised controlled trial. It may cause flushing, dyspepsia, and diarrhoea as adverse events (4). The ERA as this patient used, macitenan, has been shown to achieve a significant benefit with reduction of death, initiation of prostanoids or worsening of PAH by 45% (5). Common side effects of ERAs are hepatotoxicity and peripheral edema, but they are in general well tolerated. In patients who had WHO functional class III/IV, combination of prostanoids, ERA and PDE5I is usually the treatment of choice (1). Recently, the development of oral prostacyclin receptor agonist, selexipag offer another possible choice for them. In phase III GRIPHON study, the addition of selexipag could significantly reduce the risk of primary composite end point of death or complication related to PAH. Its common side effects are headache, diarrhoea, nausea and jaw pain (6). However, the improvement in mortality could not be demonstrated and so this add-on approach using selexipag is not routinely used. (1). Yet, the lady in this case did benefit from the combination of ERA, PDE5I and selexipag, as shown by improvement in WHO functional class, stabilization of symptoms and reduction of hospitalizations. She tolerated this combination without significant side effects. In reality, the cost of drugs might take into consideration when serving this kind of patients. However, recent meta-analyses also documented that combination therapy significantly reduced the risk of clinical worsening by ~35% compared with monotherapy alone (7).
In the pre-treatment era, patients with idiopathic PAH demonstrated a median survival of only two to three years (6,7). In treatment-era registries, median survival has improved to around 7 years (8). Death in PAH is typically related to progressive right heart failure, sudden cardiac death, or an intercurrent illness (most often respiratory failure) in which PAH predisposes to worse outcomes (9). Patients with PAH who experience cardiac arrest rarely have a ‘shockable’ rhythm and uncommonly survive.
Patients with PAH are expected to run a downhill course due to progressive right heart failure if left untreated. Physical symptoms including dyspnoea, fatigue and syncope can affect the daily living substantially (8,9). They can suffer sudden death from acute pulmonary hypertension crisis and chance of successful cardiopulmonary resuscitation was low (10). It is important to explore patient’s wish and goal of care in advance care planning. Moreover, the possibility of sudden death imposes a substantial psychological burden to patients. The impact on psychological, spiritual and social wellbeing is often overlooked. A cross-sectional study showed that up to one third of patients with PAH had psychological disorders, mainly depression and anxiety (11). Their carers can easily get exhausted as they need to pay extra effort in taking care of the patients. Both patients and their carers’ daily livings are profoundly affected (8). The impact on quality of life warrants early incorporation of PC. Some of the physicians might hesitate to refer to PC as they are fear of losing hope to patients. Patients and their family may turn down the offer. This can be partially explained by the patients’ lack of understanding on potential impacts of PAH. Some may still think that the referral to PC care may hinder the aggressive active treatment (12,13).
It is encouraging to see that this patient was benefited from PC service for several important aspects including her symptoms reduced, emotional stable, function status improved and hope reskilled as she wished to go home. In this case, use of combination PAH had palliative roles, just like chemotherapy and radiotherapy, for patients with terminal malignancy. Apart from maintaining functional status, it also helps improve symptoms and quality of life. More importantly, it gives ‘hope’ for the patient as to have short-term goals, e.g., home leave or discharge. Maintaining ‘hope’ for terminal patients is crucial to provide spiritual support for end of life care (10,14).
This case illustrated the success of early integrated care of cardiac and PC teams in managing a severe PAH patient with refractory symptoms and enable her to discharge home. PC is appropriate to support the needs of these patients. While her medical condition can be treated and followed by the parent team, her PC needs should be addressed by the PC team. In this case, she suffered from repeated episodes of chest discomfort and dizziness and required palliative inpatient titration of fentanyl injection by PC physicians. She had strong psycho-spiritual distress and was supported by PC nurse, clinical psychologist and pastoral worker. Our nurse also provided psychoeducation in order to reduce her fluid overload episodes (15). Her families was further cared by the trained social workers for their practical and emotional inputs. As this patient has a comorbidity of schizophrenia affective disorder, psychiatric team consultation might sometimes be necessary.
The schizoaffective disorder patients usually take antipsychotics and SSRI for their mood control, just like this patient. SSRIs, tryptophan, and lithium, which affect serotonin metabolism, have also been implicated in the development of pulmonary arterial hypertension (16). Maternal SSRI use has been identified as a potential risk factor for the development of persistent PH of the newborn, raising the possibility that SSRI exposure may actually be harmful to human pulmonary vascular development. In addition, a more recent population-based study in Canada reported a positive association between SSRI use and PAH, which was ascribed to residual confounding (17). Thus, the use of these medications should be well balanced against the condition of PAH, and sometimes they have to be stopped and switched into another alternatives.
Clinicians must take into account possible hemodynamic effects of any palliative intervention for PAH. An intervention that depresses systemic blood pressure, RV contractility, or increases RV afterload will cause a decline in cardiac output that can lead to a rapid spiral of worsening hypotension, systemic hypoperfusion, and death. Synergistic side effects may occur with palliative medications and PAH therapies. Specifically, systemic hypotension is a rare side effect of selexipag, but its occurrence may be precipitated by addition of frusemide, opioids and benzodiazepines (18). Thus, these drugs should be given and titrated cautiously. Collaborative care with the patient’s PAH care team is strongly advisable (14).
Recent recommendations from a PAH task force are in line with this, recommending an interprofessional approach focused on narrative medicine, quality of life, shared decision making, and timely access to PC (1). In PAH, the majority of advanced therapies align well with PC’s goal of improving quality of life and symptom burden. However, they may pose a challenge when navigating optimal symptom management due to frequent medication side effects, burdens of administration (especially with parenteral prostanoids) and potential drug-drug interactions (Table 1).

Full table
In conclusion, this case highlighted how a patient still receiving active PAH-specific therapies could benefit from the integration of PC. It is crucial to promote a more proactive approach of PC referral so that patient’s suffering can be addressed earlier (19,20). Because of limited survival for this group of patients, the cost might not be an important factor for prescribing these medications.
Acknowledgments
We would like to thank all the medical and nursing staff involving the care of this patient in Cardiac Medical Unit and Palliative Medical Unit of Grantham Hospital.
Funding: None.
Footnote
Reporting Checklist: The authors have completed the CARE reporting checklist. Available at http://dx.doi.org/10.21037/acr-20-108
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/acr-20-108). The authors have no conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee(s) and with the Helsinki Declaration (as revised in 2013). Written informed consent was obtained from the patient.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Klinger JR, Elliot CG, Levine DJ, et al. Therapy for pulmonary arterial hypertension in adults: Update of the CHEST guidelines and expert panel report. Chest 2019;155:565-86. [Crossref] [PubMed]
- Task Force for Diagnosis and Treatment of Pulmonary Hypertension of European Society of Cardiology (ESC). European Respiratory Society (ERS); International Society of Heart and Lung Transplantation (ISHLT), et al. Guidelines for the diagnosis and treatment of pulmonary hypertension. Eur Respir J 2009;34:1219-63. [Crossref] [PubMed]
- Benza RL, Miller DP, Barst RJ, et al. An evaluation of long-term survival from time of diagnosis in pulmonary arterial hypertension from the REVEAL Registry. Chest 2012;142:448-56. [Crossref] [PubMed]
- Galiè N, Ghofrani HA, Torbicki A, et al. Sildenafil citrate therapy for pulmonary arterial hypertension. N Engl J Med 2005;353:2148-57. [Crossref] [PubMed]
- Pulido T, Adzerikho I, Channick RN, et al. Macitentan and morbidity and mortality in pulmonary arterial hypertension. N Engl J Med 2013;369:809-18. [Crossref] [PubMed]
- Sitbon O, Channick R, Chin KM, et al. Selexipag for the Treatment of Pulmonary Arterial Hypertension. N Engl J Med 2015;373:2522-33. [Crossref] [PubMed]
- Lajoie AC, Lauzière G, Lega JC, et al. Combination therapy versus monotherapy for pulmonary arterial hypertension: a meta-analysis. Lancet Respir Med 2016;4:291-305. [Crossref] [PubMed]
- Guillevin L, Armstrong I, Aldrighetti R, et al. Understanding the impact of pulmonary arterial hypertension on patients' and carers' lives. Eur Respir Rev 2013;22:535-42. [Crossref] [PubMed]
- Rich S, Dantzker DR, Ayres SM, et al. Primary pulmonary hypertension. A national prospective study. Ann Intern Med. 1987;107:216-23. [Crossref] [PubMed]
- Hoeper MM, Galié N, Murali S, et al. Outcome after cardiopulmonary resuscitation in patients with pulmonary arterial hypertension. Am J Respir Crit Care Med 2002;165:341-4. [Crossref] [PubMed]
- Löwe B, Gräfe K, Ufer C, et al. Anxiety and depression in patients with pulmonary hypertension. Psychosom Med 2004;66:831-6. [Crossref] [PubMed]
- Fenstad ER, Shanafelt TD, Sloan JA, et al. Physician attitudes toward palliative care for patients with pulmonary arterial hypertension: results of a cross-sectional survey. Pulm Circ 2014;4:504-10. [Crossref] [PubMed]
- Cheung KC, Lau VW, Un KC, et al. Advance care planning for patients with advanced neurology diseases. Ann Palliat Med 2018;7:349-54. [Crossref] [PubMed]
- Christiansen D, Porter S, Hurlburt L, et al. Pulmonary Arterial Hypertension: A Palliative Medicine Review of the Disease, Its Therapies, and Drug Interactions. J Pain Symptom Manage 2020;59:932-43. [Crossref] [PubMed]
- Chan KY, Yip T, Yap DYH, et al. A Pilot Comprehensive Psychoeducation Program for Fluid Management in Renal Palliative Care Patients: Impact on Health Care Utilization. J Palliat Med 2020;23:1518-24. [Crossref] [PubMed]
- McGee M, Whitehead N, Martin J, et al. Drug-associated pulmonary arterial hypertension. Clin Toxicol (Phila) 2018;56:801-9. [Crossref] [PubMed]
- Sadoughi A, Roberts KE, Preston IR, et al. Use of selective serotonin reuptake inhibitors and outcomes in pulmonary arterial hypertension. Chest 2013;144:531-41. [Crossref] [PubMed]
- Drugs for treatment of pulmonary arterial hypertension. Available online: https://www.accessdata.fda.gov/drugsatfda_docs/label/2015/207947s000lbl.pdf
- Chan KY, Yip T, Yap DY, et al. Enhanced Psychosocial Support for Caregiver Burden for Patients With Chronic Kidney Failure Choosing Not to Be Treated by Dialysis or Transplantation: A Pilot Randomized Controlled Trial. Am J Kidney Dis 2016;67:585-92. [Crossref] [PubMed]
- Chan KY, Yap DYH, Yip T, et al. Palliative Care Consultation in Advanced Chronic Kidney Disease with Pain. J Palliat Med 2018;21:809-14. [Crossref] [PubMed]
Cite this article as: Wong CY, Tsang KW, Li CW, Au HY, Chan KY. Roles of specific drug therapies for severe pulmonary arterial hypertension in palliative care: a case report. AME Case Rep 2021;5:7.



