Sacral fatigue fracture in a young girl with no history of trauma or reported athletic activity: a case report
Introduction
Sacral fatigue fractures are infrequent in children compared with sacral insufficiency fractures in elderly patients with underlying osteoporosis (1-4). Sacral fatigue fractures in the young population usually occur from repetitious physical strain due to vigorous athletic activity. Most of these patients are teenagers, and it is an extremely rare occurrence in those younger than 13 years without a history of intense sports activity (5,6). Herein we report a case of sacral fatigue fracture in a young girl with no history of trauma or reported athletic activity. This case report is presented in accordance with the CARE reporting checklist (available at http://dx.doi.org/10.21037/acr-20-41).
Case presentation
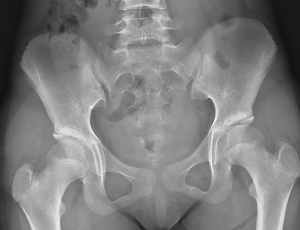
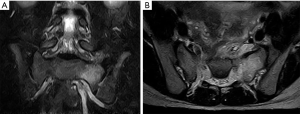
A healthy 11-year-old girl suffered sudden low back pain after standing up from the ground while on a short break in her regular physical education running class at school. Three days after onset, she visited a clinic for the constant low back pain and was treated by physical massage with no detection of any specific abnormality. She completed a 1.8-km run the same day. Soon after running, her low back pain worsened, and she visited our orthopaedic clinic the next day. She had no history of regular sports activity or notable medical history. At this visit, she was unable to walk independently without limping on the left leg. Neurological examination revealed a positive straight leg raising test with associated left buttock pain at 80 degrees on the left side with no abnormal motor or sensory findings. Radiological examination showed no obvious fractures of the lumbar vertebrae or pelvis (Figure 1). Magnetic resonance imaging (MRI) demonstrated high signal intensity changes on the short tau inversion recovery (STIR) image of the left ala, indicating bone marrow edema (Figure 2). There were no abnormal MRI findings in the lumbar spine. Thus, we diagnosed sacral fatigue fracture in the left ala and prescribed home rest. She was allowed only minimal walking with a crutch under endurable pain for 4 weeks. Her low back pain decreased with time over 3 weeks, and after 4 weeks, she was able to walk independently without gait pain. At 6 weeks, she reported no pain, and we allowed her to return to school with no restriction of physical activities. Follow-up radiological examination showed no obvious osteosclerotic change in pelvis at 6 weeks.
Written informed consent was obtained from the patient for publication of this case report and any accompanying images. A copy of the written consent is available for review by the Editor-in-Chief of the journal.
Discussion
Whether traumatic or non-traumatic, sacral fractures in children are uncommon. A previous report in 2004 presented eight cases of pediatric sacral fractures in children ranging from 1.8 to 17 years of age (7). This study included only traumatic fractures (e.g., due to motor vehicle accident or fall) and found that the sacral fractures occurred at the ala in 6 of the 8 cases. This location corresponds to zone one by the classification of Denis in which nerve root damage is occasionally associated (8).
In non-traumatic fractures, sacral stress fractures are divided into two types, sacral insufficiency fractures and sacral fatigue fractures (4,5,6,9). Patients who develop sacral insufficiency fractures are typically elderly osteoporotic females, rheumatoid arthritis sufferers treated undergoing long-term corticosteroid therapy, or cancer patients receiving pelvic radiation therapy (4). In contrast, the main risk factors for sacral fatigue fractures include a recent increase in training intensity, long distance running or a deficient diet in the adolescent age group. The mean age typically reported for sacral fatigue fractures is in the 20s and 30s (1,2,4). Thus, the fracture in our 11-year-old patient with no history of trauma or repetitious sports activity is quite rare. Hama et al. previously reported two cases of 9-year-old children with sacral fatigue fractures and mentioned that there had been only five case reports of these fractures in children aged 12 years or younger in the literature before 2016 (5). They also suggested that spina bifida occulta in the sacrum might affect the intensity of stress forces on the sacral alae in their study. Similarly, we speculate that in our patient the concentration of vertical stress forces resulting from sudden standing were dissipated from the spine to the sacral alae via the lumbosacral ligament, as previously suggested (1,2). Since our patient had no history of osteoporotic conditions, this sacral stress fracture may have occurred spontaneously.
For diagnosis of sacral fatigue fractures, plain radiographs act as the initial screening tool to rule out more common pathological conditions; however, they are usually negative for sacral fatigue fractures (2,9). In our case, even after 6 weeks, this fracture was not evidenced by obvious callus formation or bone healing consolidation in the ala. Computed tomography (CT) can demonstrate acute fracture lines and linear bands of sclerosis parallel to the sacroiliac joint in sacral stress fractures; however, fracture lines may not always be visualized, and sclerosis may not be detected during the acute phase after fracture (2,9). We did not perform a CT examination due to the risk of radiation exposure in our child patient. Although a bone scan with technetium-99m medronate methylene diphosphonate is the most sensitive technique for detecting fracture, it is not specific (1,2,4). Furthermore, since it carries the risk of radiation exposure, we do not recommend using this scan in a child. MRI is therefore considered the gold standard examination due to its high sensitivity and specificity for sacral fatigue fractures (2,4,5,9). A STIR image can significantly enhance this sensitivity by detecting bone marrow edema, and coronal views can support visualization of the extent and location of the fractures (4,9). Coronal views also provide information on whether the fractures exist at sacral neural foramina which may indicate the possibility of neurological deficits resulting from the fracture (4,9). According to a previous report by Denis, sacral fractures are associated with a 32% incidence of neurological deficits, and nerve root damage is present in 5.9% of cases when fractures were in zone one, 28% in zone two, and 87% in zone three (7). Since most of the sacral fatigue fractures occur in zone one, patients may recover over time without any neurological deterioration. Thus, we speculate that sacral fatigue fractures in children may be more common than expected; most physicians who are not familiar with this type of fracture are apt to misdiagnose it.
In conclusion, we report a case of spontaneous pediatric sacral fatigue fracture in an 11-year-old patient with no history of trauma. MRI is extremely valuable for the diagnosis of this fracture. We should consider the possibility of sacral fatigue fractures when we treat young patients with a chief complaint of unexplained low back pain.
Acknowledgments
Funding: None.
Footnote
Reporting Checklist: The authors have completed the CARE reporting checklist. Available at http://dx.doi.org/10.21037/acr-20-41
Conflicts of Interest: Both authors have completed the ICMJE uniform disclosure form(available at http://dx.doi.org/10.21037/acr-20-41). The authors have no conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee(s) and with the Helsinki Declaration (as revised in 2013). Written informed consent was obtained from the patient for publication of this case report and any accompanying images. A copy of the written consent is available for review by the Editor-in-Chief of the journal.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Micheli LJ, Curtis C. Stress fractures in the spine and sacrum. Clin Sports Med 2006;25:75-88. ix. [Crossref] [PubMed]
- Patterson SP, Daffner RH, Sciulli RL, et al. Fatigue fracture of the sacrum in an adolescent. Pediatr Radiol 2004;34:633-5. [Crossref] [PubMed]
- Shah MK, Stewart GW. Sacral stress fractures: an unusual cause of low back pain in an athlete. Spine (Phila Pa 1976) 2002;27:E104-8. [Crossref] [PubMed]
- Yoder K, Bartsokas J, Averell K, et al. Risk factors associated with sacral stress fractures: a systematic review. J Man Manip Ther 2015;23:84-92. [Crossref] [PubMed]
- Hama S, Takata Y, Sakai T, et al. Sacral fatigue fractures in children with sacral spina bifida occulta. J Pediatr Orthop B 2016;25:278-82. [Crossref] [PubMed]
- Lam KS, Moulton A. Stress fracture of the sacrum in a child. Ann Rheum Dis 2001;60:87-8. [Crossref] [PubMed]
- Hart DJ, Wang MY, Griffith P, et al. Pediatric sacral fractures. Spine (Phila Pa 1976) 2004;29:667-70. [Crossref] [PubMed]
- Denis F, Davis S, Comfort T. Sacral fractures: an important problem. Retrospective analysis of 236 cases. Clin Orthop Relat Res 1988.67-81. [PubMed]
- Zaman FM, Frey M, Slipman CW. Sacral stress fractures. Curr Sports Med Rep 2006;5:37-43. [Crossref] [PubMed]
Cite this article as: Nomura H, Nomura S. Sacral fatigue fracture in a young girl with no history of trauma or reported athletic activity: a case report. AME Case Rep 2020;4:27.