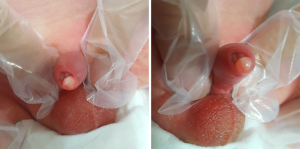
Neonate with a parameatal urethral cyst
Introduction
Parameatal urethral cyst is an ultra rare condition, and only a few cases have been reported in the literature (1-12). This cyst can be present at birth, or develop any time during childhood, although they usually manifest during the first year of life (4). Here, we report a neonate with a parameatal urethral cyst without symptoms and review the previous reports on parameatal urethral cysts.
Case presentation
At 10-hour after birth, a male neonate was referred to our urology department for a cystic lesion on the penis tip. He was born by cesarean section after 38.5 weeks of gestation, and had a body weight of 3,460 g. He was in good health, and had an Apgar score of 8 at 1 min, and 9 at 5 min. He presented with a 5×5 mm2 spherical cystic mass at the external urethral meatus on the ventral margin (Figure 1). The cyst appeared to be filled with a serous to slightly milky fluid, and was easily differentiated from a smegma pearl. The cyst was unlikely to be infected, because there were no topical or systematic signs of inflammation. Preputial skin partly covered the cystic mass, and it could not be detached by moderate tearing. The penis looked normal without hypospadias. His urine stream was good, without spraying, and the urinalysis results were normal, with no signs of infection or inflammation. He was feeding normally and the physical examination results were otherwise normal. Abdominal ultrasound showed normal kidneys and bladder. Based on a diagnosis of asymptomatic neonatal parameatal urethral cyst, we planned watchful follow-up and expected spontaneous resolution. Until 12 months follow-up, the cyst is stable in size without symptoms.
Discussion
Parameatal urethral cyst is an ultra rare condition, and only a few cases have been reported in the literature. Since Thompson and Lantin presented the first case report of parameatal urethral cyst in 1956 (2), fewer than 100 cases have been reported in worldwide (1-12). Parameatal urethral cyst may be unfamiliar to pediatricians and urologists due to its rarity. Even though most case reports described one or a few cases, there are two studies with largest number of cases that give us long-term follow-up information of parameatal urethral cyst (1,4).
Matsuyama et al. performed a long-term follow-up study of 46 patients with parameatal urethral cysts that first presented at a median age of 44 months (range, 0–140 months) (1). In their largest known study, they reported that 80% of patients were asymptomatic, and 20% had pain on urination, deflected urinary streams, difficulty with foreskin retraction, or pain from a ruptured cyst. Eighty-five percent of cysts were located on the lateroventral side of the meatus and one child had a dorsal cyst. The most common size was less than 5 mm in diameter (82.6%). Twenty-nine patients (63%) underwent surgical excision for symptoms or cosmetic reasons at a median age of 61 months. For 16 patients not receiving operations, 4 patients (25%) had spontaneous resolution, 4 (25%) improved, 7 (43.8%) stabilized and only 1 (6.3%) had enlargement of cyst. The median age of spontaneous resolution was 24 months (range, 6–110 months). Patients who initially had no symptoms continued to have no symptoms during follow-up. There was no recurrence in patients who underwent surgical excision.
Willis et al. reported a retrospective review of 18 prepubertal boys with parameatal urethral cyst (4). First presentation of the cyst was at birth or within the first year of life in 12 patients (67%). Twelve patients (67%) were asymptomatic and all were less than 1 cm and 63% were less than 5mm in diameter. Fourteen patients (78%) treated surgically underwent complete excision of the cyst, and there was no recurrence. Among 4 patients did not undergo surgical excision, 1 (6%) experienced spontaneous resolution during the first weeks of life, and the other 3 did not seek further treatment.
A parameatal urethral cyst is a benign lesion, and is mainly asymptomatic. The cysts can be present at birth or develop at any time during childhood or adulthood (11), and they can occur in female (12) as well as male, although they mostly manifest in male during the first year of life (4). The etiology of parameatal cyst is uncertain. The possible causes are persistence of cystic spaces during the process of preputial delamination (2), cyst formation from anomalous fusion of the urethra (1), or obstruction of the paraurethral duct (6).
A proportion of 66% to 80% of parameatal urethral cysts are asymptomatic, but patients may show symptoms like dysuria, voiding difficulty or urine spraying (1,4). Most of parameatal urethral cysts can be diagnosed by physical examination. A total of 91.3% to 100% of cysts are less than 1 cm in diameter (1,4) and located ventral or lateral to the meatus (6). It is important to differentiate these cysts from an epidermal inclusion cyst, a skin tag, a dermoid cyst, or a cyst located anywhere other than urethral meatus (4).
There is no standard treatment guidelines of parameatal urethral cyst due to its rarity. A parameatal urethral cyst may resolve spontaneously. Among patients who chose conservative management, 25% of patients showed spontaneous resolution (1,4). Another case report by Oka et al. described spontaneous resolution of parameatal urethral cyst in a neonate at 4 months (8). Therefore, if there is no voiding discomfort or irritative symptoms, periodic follow-up is appropriate. Periodic follow-up is supported because general anesthesia for surgical excision is associated with certain risks. But in case of symptomatic cysts like symptoms like dysuria, voiding difficulty or urine spraying, surgical excision should be considered. Surgical excision can be also performed with minimal morbidity and good cosmetic results for patients whose cysts does not resolve naturally up to 24 months, or who are concerned of cosmesis (4). There are no reports of recurrence after complete surgical excision of these cysts. But, simple aspiration or marsupialization of the cyst could lead to recurrence or unsatisfactory cosmesis, so should be avoided (7).
In our case reports, we planned watchful follow-up and expected spontaneous resolution. Until 12 months follow-up, the cyst is stable in size without symptoms. If the cyst does not resolve up to 24 months or any symptoms occur, surgical excision will be discussed with the parents.
Acknowledgments
Funding: This work was supported by the National Research Foundation of Korea (NRF) grant funded by the Korea government (MSIT) (No. 2019R1G1A1002237).
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
Informed Consent: Written informed consent was obtained from the patient’s parents for publication of this manuscript.
References
- Matsuyama S, Matsui F, Yazawa K, et al. Long-term Follow-up of Median Raphe Cysts and Parameatal Urethral Cysts in Male Children. Urology 2017;101:99-103. [Crossref] [PubMed]
- Lantin PM, Thompson IM. Parameatal cysts of the glans penis. J Urol 1956;76:753-5. [Crossref] [PubMed]
- Nam DH, Kim SO, Hwang EC, et al. Parameatal urethral cyst of the glans penis with unusual pathologic finding. Korean Journal of Pediatric Urology 2010;2:116-7.
- Willis HL, Snow BW, Cartwright PC, et al. Parameatal urethral cysts in prepubertal males. J Urol 2011;185:1042-5. [Crossref] [PubMed]
- Hill JT, Ashken MH. Parameatal urethral cysts: a review of 6 cases. Br J Urol 1977;49:323-5. [Crossref] [PubMed]
- Shiraki IW. Parametal cysts of the glans penis: a report of 9 cases. J Urol. 1975;114:544-8. [Crossref] [PubMed]
- Koga S, Arakaki Y, Matsuoka M, et al. Parameatal urethral cysts of the glans penis. Br J Urol 1990;65:101-3. [Crossref] [PubMed]
- Oka M, Nakashima K, Sakoda R. Congenital parameatal urethral cyst in the male. Br J Urol 1978;50:340-1. [Crossref] [PubMed]
- Yamada N, Yoshida Y, Ito A, et al. Three-dimensional structure of a parameatal urethral cyst by scanning electron microscopy. Urology 2013;81:1072-4. [Crossref] [PubMed]
- Yoshida K, Nakame Y, Negishi T. Parameatal urethral cysts. Urology 1985;26:490-1. [Crossref] [PubMed]
- Sinha RK, Mukherjee S, Mitra N, et al. Parameatal Cyst: A report of Two Cases and Review of Literature. Malays J Med Sci 2015;22:71-3. [PubMed]
- Soyer T, Aydemir E, Atmaca E. Paraurethral cysts in female newborns: role of maternal estrogens. J Pediatr Adolesc Gynecol 2007;20:249-51. [Crossref] [PubMed]
Cite this article as: Song SH, Kim DS. Neonate with a parameatal urethral cyst. AME Case Rep 2019;3:16.