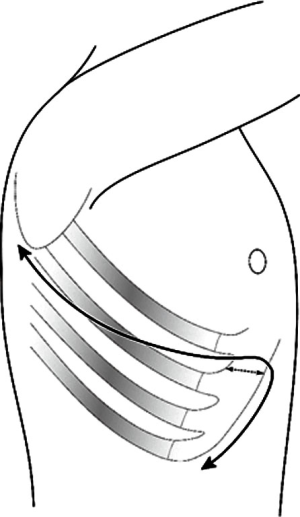
Extended thoracotomy with subcostal incision for giant solitary fibrous tumor of the diaphragm
Introduction
Solitary fibrous tumors of the pleura (SFTPs) are relatively rare, and complete resection is the preferred treatment (1). En bloc resection is necessary for giant SFTPs because an increased tumor size suggests malignant potential (2). We experienced a giant SFTP originating from the diaphragm. The patient underwent complete resection via extended posterolateral thoracotomy combined with a subcostal incision. We herein report the resection technique for giant SFTP of the diaphragm.
Case presentation
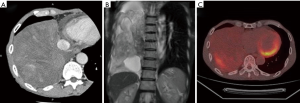
A 74-year-old asymptomatic man presented to our hospital with an abnormal chest radiograph. Computed tomography revealed an 18-cm-diameter giant mass in his right thorax (Figure 1A). A T2-weighted magnetic resonance image suggested that the tumor contained a cystic lesion (Figure 1B). No detectable malignant lesions were present in other organs. Positron emission tomography showed abnormal uptake by the tumor (Figure 1C). An ultrasonography-guided needle biopsy suggested a solitary fibrous tumor. The patient underwent surgery. A posterolateral incision was extended along the costal arch (Figure 2), and we cut the sixth cartilage. Because the tumor was located on the diaphragm and adhered to the right lower lobe of the lung, partial resection of the diaphragm and right lung was performed using a linear mechanical stapler. We also sutured and reinforced the staple line of the diaphragm. The transected sixth cartilage was fixed by synthetic absorbable suture. We achieved en bloc resection without rupturing the cystic lesion (Figure 3) (3). The postoperative course was uneventful. Pathological examination revealed a malignant solitary fibrous tumor. There were no signs of invasion of the right lung, and the surgical margin was negative. The patient developed no recurrence for 1 year postoperatively.

Discussion
We have herein reported the successful resection of a giant SFTP via extended thoracotomy with a subcostal incision. This operative technique is useful for resection of diaphragmatic tumors. The approach provides better visualization the costophrenic angle, allowing safer and more reliable surgical manipulation around the diaphragm.
Solitary fibrous tumors originating from the diaphragm are very rare. To the best of our knowledge, only five cases of SFTPs arising from the diaphragm have been described in the literature (4-8). Treatment of giant SFTPs requires complete resection (1). SFTPs are usually benign; however, large tumors are reportedly more likely to be malignant (2). A positive surgical margin is predictive of not only worse local recurrence-free survival but also worse metastasis-free survival (9). One study showed that patients with malignant SFTPs treated with incomplete resection did not survive beyond 5 years after surgery, with a striking difference from patients who underwent complete resection (10). Thus, complete en-bloc resection is necessary for the treatment of solitary fibrous tumors, especially giant SFTPs with malignant potential.
To achieve complete resection of the giant SFTP originating from the diaphragm in the present case, we made a subcostal skin incision following a posterolateral incision (Figure 2). This approach provides the surgeon a wide visual field for the costophrenic angle, allowing safer and more reliable surgical manipulation around the diaphragm. This procedure is useful for complete resection of tumors arising from the diaphragm. Moreover, our surgical approach also has an advantage in pulmonary resection. When additional pulmonary resection is needed, the skin incision can be extended dorsally. Extending the posterior thoracotomy dorsally makes it easy to perform pulmonary resection procedures such as lobectomy.
Our surgical approach differs from lower door open (LDO) thoracotomy (11). Our procedure involves transection of only one costal cartilage, whereas LDO thoracotomy requires transection of five cartilages. We consider that fixation of the costal cartilage is easier in our surgical procedure than in LDO thoracotomy. Mild paradoxical respiratory movement is seen after LDO thoracotomy (12). However, our patient did not experience paradoxical respiratory movement because we only cut one cartilage, and our procedure does not affect postoperative thoracic movement. LDO thoracotomy is useful for extrapleural pneumonectomy because it requires reconstruction of the diaphragmatic and pericardial defects. In the present case, we only performed direct suturing following mechanical suturing for the diaphragm; no reconstruction was needed. Thus, our surgical approach is appropriate for giant SFTPs of the diaphragm.
In conclusion, extended thoracotomy with a subcostal incision is an effective surgical approach for surgical removal of giant tumors originating from the diaphragm.
Acknowledgements
We thank Angela Morben, DVM, ELS, from Edanz Group (www.edanzediting.com/ac) for editing a draft of this manuscript.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
Informed Consent: Written informed consent was obtained from the patient to publish this manuscript and any accompanying images.
References
- Chick JF, Chauhan NR, Madan R. Solitary fibrous tumors of the thorax: nomenclature, epidemiology, radiologic and pathologic findings, differential diagnoses, and management. AJR Am J Roentgenol 2013;200:W238-48. [Crossref] [PubMed]
- Harrison-Phipps KM, Nichols FC, Schleck CD, et al. Solitary fibrous tumors of the pleura: results of surgical treatment and long-term prognosis. J Thorac Cardiovasc Surg 2009;138:19-25. [Crossref] [PubMed]
- Yanagiya M, Matsumoto J, Miura T, et al. Surgical removal of a giant solitary fibrous tumor of the pleura originating in the diaphragm. Asvide 2017;4:521. Available online: http://www.asvide.com/articles/1843
- Ge W, Yu DC, Jiang CP, et al. Giant solitary fibrous tumor of the diaphragm: a case report and review of literature. Int J Clin Exp Pathol 2014;7:9044-9. [PubMed]
- Norton SA, Clark SC, Sheehan AL, et al. Solitary fibrous tumour of the diaphragm. J Cardiovasc Surg (Torino) 1997;38:685-6. [PubMed]
- Ota H, Kawai H, Yagi N, et al. Successful diagnosis of diaphragmatic solitary fibrous tumor of the pleura by preoperative ultrasonography. Gen Thorac Cardiovasc Surg 2010;58:485-7. [Crossref] [PubMed]
- Hunt I, Ewanowich C, Reid A, et al. Managing a solitary fibrous tumour of the diaphragm from above and below. ANZ J Surg 2010;80:370-1. [Crossref] [PubMed]
- Kita Y. Pleural solitary fibrous tumor from diaphragm, being suspected of liver invasion; report of a case. Kyobu Geka 2012;65:338-40. [PubMed]
- Gold JS, Antonescu CR, Hajdu C, et al. Clinicopathologic correlates of solitary fibrous tumors. Cancer 2002;94:1057-68. [Crossref] [PubMed]
- Lococo F, Cesario A, Cardillo G, et al. Malignant solitary fibrous tumors of the pleura: retrospective review of a multicenter series. J Thorac Oncol 2012;7:1698-706. [Crossref] [PubMed]
- Horio H, Nomori H. Thoracotomy technique for extrapleural pneumonectomy in treatment of diffuse pleural mesothelioma. J Jap Assoc Chest Surg 1995;9:538-41. [Crossref]
- Yoshioka M, Nomori H, Mori T, et al. Extrapleural pneumonectomy via a lower door open thoracotomy with reconstruction of the diaphragm and pericardium using autologous materials for mesothelioma. Surg Today 2006;36:1036-8. [Crossref] [PubMed]
Cite this article as: Yanagiya M, Matsumoto J, Miura T, Horiuchi H. Extended thoracotomy with subcostal incision for giant solitary fibrous tumor of the diaphragm. AME Case Reports 2017;1:8.